Affiliated Foot Care Center
Call 860•349•8500 or 203•294•4977
An ulcer is a sore on the skin or a mucous membrane, accompanied by the disintegration of tissue.
The wounds from which ulcers arise can be caused by a wide variety of factors, but the main cause is impaired blood circulation. Especially, chronic wounds and ulcers are caused by poor circulation, either through cardiovascular issues or external pressure from a bed or a wheelchair.
A very common and dangerous type of skin ulcers are caused by what are called pressure-sensitive sores, more commonly called bed sores and which are frequent in people who are bedridden or who use wheelchairs for long periods. Other causes producing skin ulcers include bacterial or viral infections, fungal infections and cancers. Blood disorders and chronic wounds can result in skin ulcers as well.
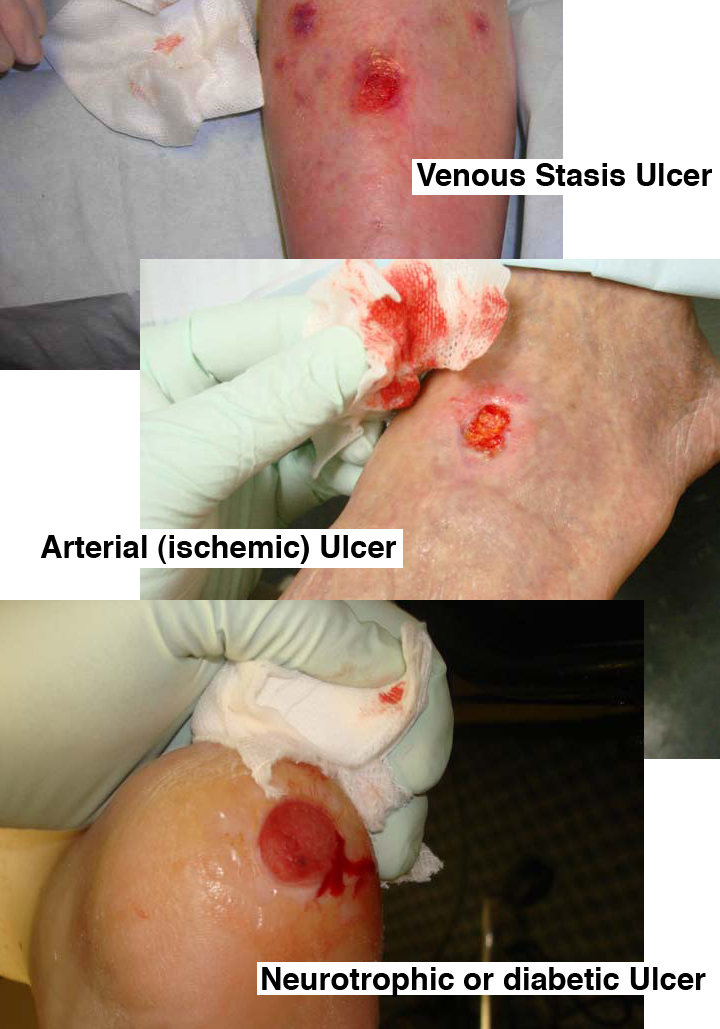
There are three common kinds of leg and foot ulcers, defined by appearance, location and the way the borders and skin around the ulcer look.
Venous Stasis ulcers are located below the knee and are primarily found on the inner part of the leg, just above the ankle.
The base of a venous ulcer is usually red but it may also be covered with yellow fibrous tissue or there may be a green or yellow discharge if you have an infection. This kind of ulcer can drain a lot of fluid and you will notice that on your clothing.
The borders of a venous ulcer are irregular and the skin around it is frequently discolored and swollen. It may even feel warm to the touch. The skin may appear shiny and tight, depending on how much swelling you have. It may also be discolored and look brown or purple. If you have had a history of swollen legs or chronic problems with varicose veins or blood clots in your lower legs you will have a tendency to get venous stasis ulceration.
Arterial (ischemic) ulcers are usually on your heels, tips of your toes, between your toes where they rub against one another. They can also occur anywhere your bones protrude and rub against your socks or shoes. They can also occur in your nail bed if your toenail cuts into the skin or if you trim your nails too short of if you have had an ingrown toenail removed.
The arterial or ischemic ulcer has a yellow, brown, gray, or blackened color and usually does not bleed. The borders and surrounding skin usually appear as though they have been punched out. If the ulcer is irritated or infected, there may or may not be swelling and redness around the base of the ulcer. Your entire foot may turn red when you dangle your leg and this redness often turns pale white and yellow when you raise your leg.
These ulcers usually are very painful, especially at night. You may be in the habit of dangling your foot over the side of your bed to get comfortable when you sleep. You may also be aware that you have poor leg circulation due to previous doctor visits.
Neurotrophic or diabetic ulcers may occur at pressure points on the bottom of your feet but they can occur anywhere on your feet where they have been injured. You can get these ulcers if you have diabetes or any condition that reduces the feeling in your feet.
This kind of ulcer will look differently depending on how much circulation you have in your feet.. It it can be pink and or red or brown or black. The borders of the ulcer are punched out, while the skin around the ulcer is calloused from repeated rubbing against your shoe or another part of your foot.
These ulcers happen frequently in people with lack of sensation in their feet due to nerve damage. This kind of damage causes changes in the sweat glands in your feet as well as lack of feeling in your feet. As a result, you won't notice cracking of your skin, calluses or blistering due to friction. If you have neuropathy, you may notice numbness, tingling or burning sensations in your feet.
It is easy to understand why people with diabetes are more prone to foot ulcers than anyone else. If you have diabetes, you need to regularly inspect your feet for any problems and call us for a complete checkup every nine weeks. You should never go barefoot.
Dr Fosdick has found that ulcers very rapidly disappear when treated using laser therapy. If you have an ulcer that won't go away, see Dr. Fosdick immediately!